Wisdom teeth have long sparked debates in dentistry and popular culture, with many assuming that extraction is an automatic necessity. These third molars emerge later than other teeth, often during late adolescence or early adulthood, and their arrival has been historically associated with discomfort, crowding, or potential oral health issues. Yet, the question remains complex: do all wisdom teeth truly require removal, or are there circumstances in which they can coexist harmlessly with the rest of the dentition? Understanding this topic requires a nuanced approach that combines anatomy, dental research, and evolving perspectives in preventive care.
Table Of Contents
- The Anatomy and Function of Wisdom Teeth
- Common Challenges Associated with Wisdom Teeth
- Radiographic Insights and Predictive Assessment
- Risk Factors and Potential Complications of Wisdom Teeth
- Age and Timing Considerations for Wisdom Teeth
- Symptomatic vs. Asymptomatic Wisdom Teeth
- Cultural and Geographic Variations in Wisdom Teeth Management
- Advances in Imaging and Predictive Technology
- Post-Extraction Considerations and Recovery Insights
- Long-Term Perspectives on Retaining Wisdom Teeth
- Scientific Debates and Evolving Guidelines
- Anatomical Variability and Impaction Patterns
- Functional and Aesthetic Considerations
- Cultural, Social, and Policy Perspectives
- Integrating Science, Observation, and Individualized Care
The Anatomy and Function of Wisdom Teeth
Wisdom teeth represent the third set of molars in the human mouth, usually positioned at the very back of the jaw. Unlike the first and second molars, their eruption occurs later, which sometimes limits available space for proper alignment. Interestingly, anthropologists note that our ancestors often had larger jaws, making room for these teeth without complications. Today, however, reduced jaw size in modern populations can create variability in eruption patterns and positioning.
From a functional perspective, wisdom teeth are capable of aiding in chewing and overall dental load distribution when they erupt fully and align correctly. In some individuals, these teeth integrate seamlessly, showing normal morphology and alignment. Yet, this potential utility must be weighed against the frequent complications that can arise when space is restricted, such as impaction or difficulty cleaning. This dual role highlights the complexity behind decisions regarding their management.
Common Challenges Associated with Wisdom Teeth
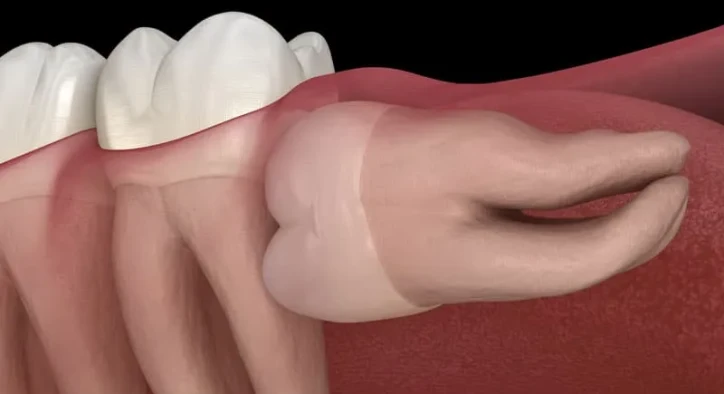
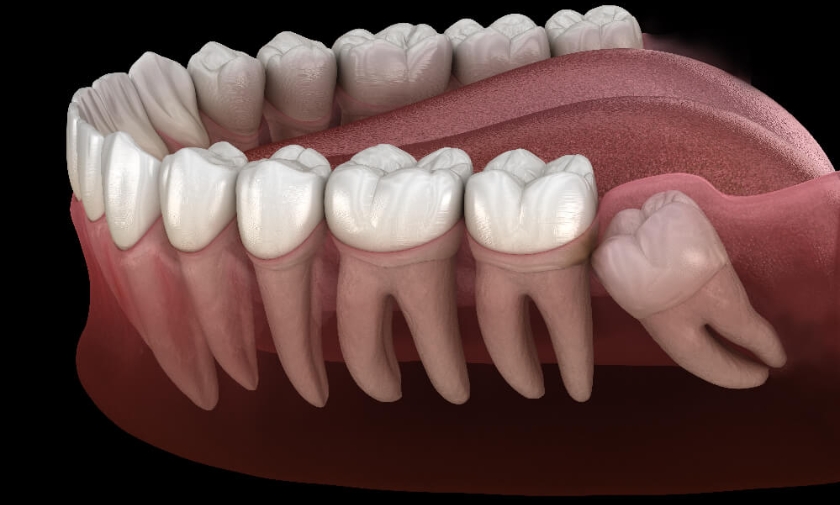
Wisdom teeth can present challenges even when fully erupted. One of the primary concerns is partial eruption, where the tooth only emerges partially through the gum. This scenario can create pockets that trap bacteria, potentially leading to localized inflammation or infection. Additionally, angulated or misaligned wisdom teeth can exert pressure on neighboring teeth, sometimes contributing to crowding or discomfort.
Beyond mechanical concerns, impacted wisdom teeth teeth that fail to emerge completely can increase the risk of cyst formation or enamel resorption in adjacent molars. Researchers have also observed a correlation between specific eruption patterns and oral microbiome changes in the posterior region of the mouth. While not every individual experiences these issues, such findings emphasize that wisdom teeth management should be tailored, informed by anatomy, imaging, and careful monitoring.
Radiographic Insights and Predictive Assessment
Wisdom teeth are often evaluated using panoramic radiographs or cone-beam CT imaging to determine position, angulation, and potential interactions with surrounding structures. Radiographic analysis allows dentists to identify whether a tooth is likely to erupt normally, remain impacted, or interfere with adjacent teeth. This predictive approach helps balance the risks and benefits of extraction versus retention.
The assessment also extends to evaluating nerve proximity, root morphology, and bone density. Certain patterns, such as horizontal impaction or proximity to the inferior alveolar nerve, can complicate potential removal and influence the clinical recommendation. Scientific literature suggests that individualized imaging and longitudinal observation provide the most accurate basis for making informed decisions, rather than applying blanket extraction protocols.
Risk Factors and Potential Complications of Wisdom Teeth
Wisdom teeth can introduce risk factors beyond the common discomfort associated with eruption. One frequent concern is pericoronitis, an inflammatory condition affecting partially erupted teeth. In these cases, the gum tissue around the tooth can trap food debris and bacteria, potentially leading to swelling, pain, or infection. Although not everyone develops these symptoms, such localized reactions are among the most cited reasons for extraction.
Other potential complications include crowding of adjacent teeth and damage to the roots or enamel of neighboring molars. Researchers note that even asymptomatic wisdom teeth may exert subtle pressure that over time contributes to misalignment, although the degree of effect varies by individual anatomy. Additionally, cysts or rare benign growths can form around impacted third molars, creating further motivation to assess each tooth carefully rather than assuming a universal approach.
Age and Timing Considerations for Wisdom Teeth
Wisdom teeth present unique considerations related to age and skeletal development. Young adults often have more flexible bone structures, which can make extraction procedures simpler and recovery faster if removal is necessary. Conversely, delaying intervention into later adulthood may coincide with denser bone and more complex root formations, potentially complicating surgical procedures.
Research has shown that eruption patterns also correlate with age. Teeth that emerge earlier in the late teens may align more favorably, while delayed eruption sometimes increases the likelihood of impaction or angulation problems. Age-related evaluation provides dentists with an important framework for determining whether proactive monitoring or removal is advisable.
Symptomatic vs. Asymptomatic Wisdom Teeth
Wisdom teeth are not uniformly problematic; some erupt fully and remain asymptomatic for years. Individuals with well-aligned third molars often experience minimal interference with oral function and may not require extraction at all. These asymptomatic cases highlight that blanket removal is not always necessary and that individualized assessment is critical.
Conversely, symptomatic teeth those causing pain, recurrent infection, or structural compromise typically warrant more attention. Clinical evaluation considers both immediate symptoms and potential future risks. This approach emphasizes that treatment decisions should be informed by a combination of current presentation, anatomical analysis, and predictive risk modeling.
Cultural and Geographic Variations in Wisdom Teeth Management
Wisdom teeth management practices vary widely across cultures and healthcare systems. In some countries, prophylactic removal of third molars is routine, driven by historical clinical guidelines and preventive strategies. Elsewhere, more conservative approaches prevail, relying on monitoring and intervention only when symptoms arise or radiographic evidence indicates risk.
These differences provide insight into how perception, policy, and evidence influence dental practice. Comparative studies suggest that outcomes can be favorable with both strategies when applied judiciously, underscoring that individualized assessment remains a cornerstone of responsible care. Population-based research also reveals variations in jaw morphology and eruption tendencies, suggesting that what is routine in one group may be unnecessary in another.
Advances in Imaging and Predictive Technology
Wisdom teeth evaluation has benefited greatly from advances in imaging technology. Cone-beam CT scans, digital panoramic radiographs, and 3D modeling allow clinicians to visualize tooth position, angulation, and relation to nerves with unprecedented precision. This enhanced visibility supports predictive assessment of eruption potential and informs whether surgical intervention is advisable.
Technology also enables longitudinal tracking. By comparing scans over time, clinicians can detect changes in tooth orientation, root development, or jaw alignment. These observations help identify patterns that might indicate future complications, allowing for timely intervention while avoiding unnecessary procedures in teeth that are likely to erupt without incident.
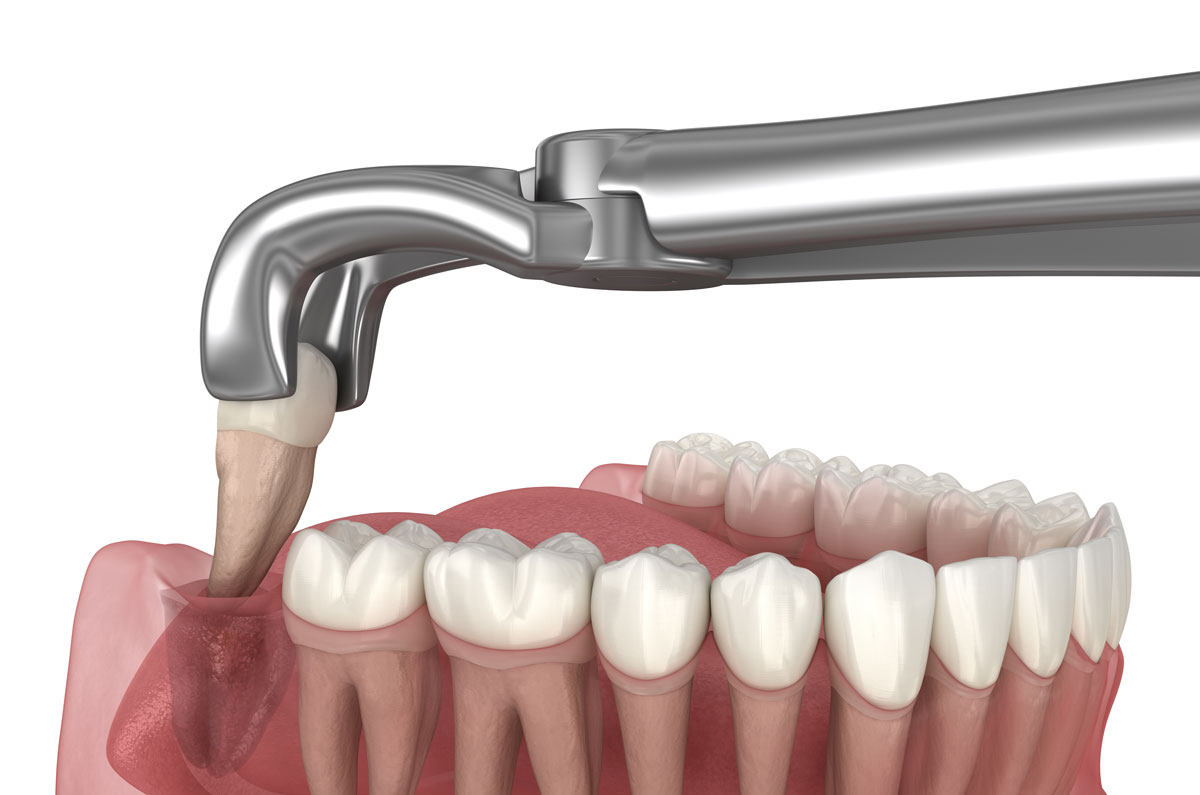
Post-Extraction Considerations and Recovery Insights
Wisdom teeth extraction, when necessary, is often followed by considerations related to healing, oral function, and bone remodeling. Recovery involves monitoring tissue repair, managing swelling, and ensuring that surrounding teeth remain unaffected. Research has highlighted that younger patients generally experience faster healing due to more adaptable bone and soft tissue structures.
Long-term observations also suggest that early removal may prevent crowding or cyst formation in some cases. However, surgical intervention is not without temporary disruption. Knowledge of typical recovery patterns helps contextualize risks and allows patients and clinicians to weigh potential benefits against the invasiveness of the procedure. Recovery data reinforces that wisdom teeth management is both anatomical and strategic, reflecting the interplay between function, risk, and timing.
Long-Term Perspectives on Retaining Wisdom Teeth
Wisdom teeth that remain in place without causing symptoms offer valuable insight into long-term oral health considerations. Longitudinal studies suggest that a subset of individuals can retain their third molars well into adulthood without notable complications. These cases demonstrate that teeth can erupt fully, align properly, and coexist with neighboring molars, providing functional chewing surfaces without interfering with overall dental integrity.
Researchers also observe that careful monitoring of retained wisdom teeth can prevent sudden complications. Regular dental checkups allow clinicians to detect early signs of misalignment, decay, or soft tissue issues. This proactive approach illustrates that non-extraction does not equate to neglect; rather, it reflects a tailored strategy that prioritizes individual anatomy and risk profiles over routine removal.
Scientific Debates and Evolving Guidelines
Wisdom teeth management continues to generate debate within dental research. Early guidelines often advocated prophylactic removal for most young adults, citing the potential for future problems. Contemporary perspectives, however, increasingly favor selective intervention based on symptomatology, imaging data, and predictive assessment.
Meta-analyses highlight the need for nuanced decision-making. While some teeth may pose minimal risk, others may threaten adjacent structures, lead to infection, or contribute to crowding. These findings reinforce the importance of individualized evaluation, bridging clinical observation, patient history, and radiographic evidence to determine whether extraction is appropriate or whether retention remains safe.
Anatomical Variability and Impaction Patterns
Wisdom teeth display wide anatomical variability, which influences management decisions. Teeth may erupt vertically, horizontally, or at varying angles, with root complexity and jawbone density affecting potential complications. Horizontal impactions, for example, often have a higher risk of damaging neighboring teeth, whereas vertically aligned molars may remain asymptomatic indefinitely.
Understanding these patterns allows clinicians to anticipate likely outcomes and personalize treatment strategies. Variability also provides an opportunity for researchers to explore correlations between craniofacial development, eruption timing, and long-term dental stability, creating a richer scientific context for decision-making.
Functional and Aesthetic Considerations
Wisdom teeth can contribute to overall occlusion and chewing efficiency when fully erupted and properly aligned. In some cases, these teeth complete the dental arch, supporting functional load distribution during mastication. Conversely, impacted or malaligned third molars may disrupt occlusion or create areas difficult to clean, which can indirectly affect oral aesthetics.
Aesthetic considerations are increasingly recognized in modern dentistry, particularly when wisdom teeth influence smile symmetry or alignment. While not the primary reason for extraction, these factors complement functional and risk assessments, demonstrating that wisdom teeth management encompasses both scientific and perceptual dimensions.
Cultural, Social, and Policy Perspectives
Wisdom teeth removal practices vary significantly across cultures and healthcare systems. In some regions, early extraction is standard preventive care, while others adopt a more conservative approach emphasizing observation and symptom-driven intervention. These variations highlight the role of cultural norms, insurance policies, and professional guidelines in shaping decisions.
Social perception also influences patient expectations. Many adults assume removal is inevitable based on familial advice, peer experiences, or public information. Addressing these assumptions requires clear communication about individualized risk, anatomical variation, and the evidence supporting selective versus routine extraction strategies.
Integrating Science, Observation, and Individualized Care
Wisdom teeth illustrate the intersection of anatomy, predictive science, and clinical judgment. They are neither universally harmful nor inherently harmless; outcomes depend on structural alignment, eruption patterns, and individual risk factors. Integrating radiographic assessment, patient history, and longitudinal monitoring allows for informed, nuanced decisions rather than default extraction.
In conclusion, wisdom teeth management exemplifies the importance of personalized evaluation. Some teeth may necessitate removal due to impaction, infection, or functional interference, while others can remain safely within the dental arch. Scientific observation, technological advancements, and awareness of individual anatomical variability collectively inform an approach that balances safety, function, and long-term oral health, moving beyond blanket assumptions toward evidence-based, patient-centered care.